We believe we’ve entered a new equilibrium with the pandemic, as most people have had the virus or are vaccinated by now. And that any rises in cases going forward should be driven by seasonality, waning immunity, and/or new variants. Top viral surveillance insights below:
- Subvariants of concern plateauing in frequency: The Omicron subvariants that most were concerned with – BA.5 and BA.4 – are peaking and flattening out. BA.4.6, which the CDC started monitoring separately, is gradually increasing in frequency, and is at 6% of all sequences. BA.2.75 is still at <1% in our data.
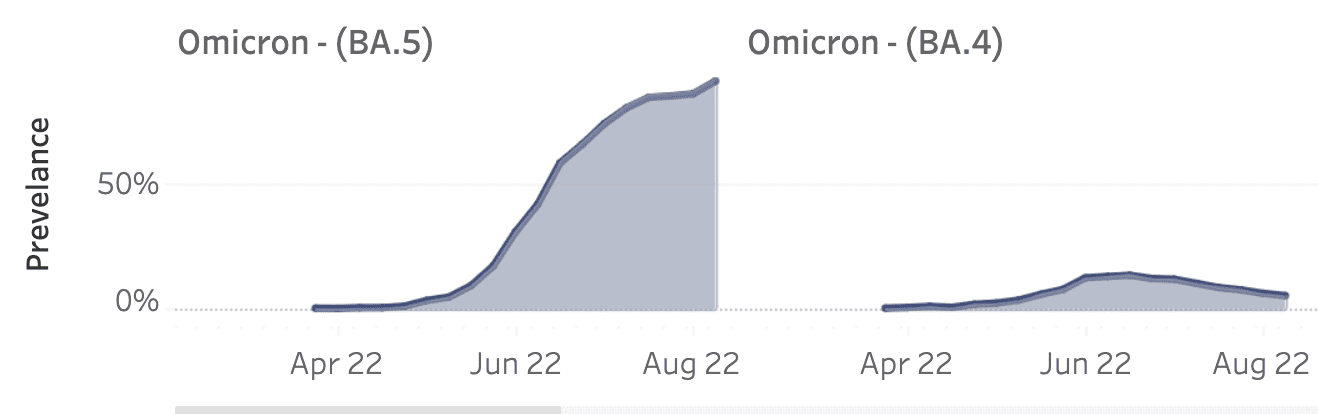
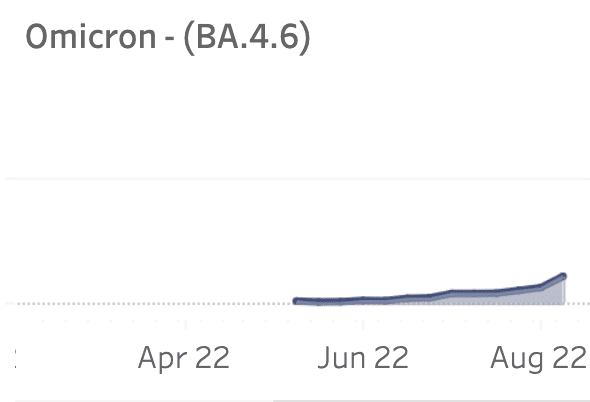
- While COVID test positivity is still high at ~30%, it’s likely due to a decrease in testing among asymptomatic cases: “Regular testers” in our data – or those who test on average almost every week, possibly as part of a workplace or school program – only have a positivity rate of ~5%, which is ~6 fold lower. As a lot of testing has moved to antigen, 5% (or 1 in 20 people) is more likely an accurate reflection of true positivity in the U.S.
- COVID cases for individuals <18 years old are rising: The rise is happening sooner than expected, as most schools are just re-opening. But we’ll keep an eye on it, as well as, flu, which we still predict will see a spike this fall (though we have not seen it yet).
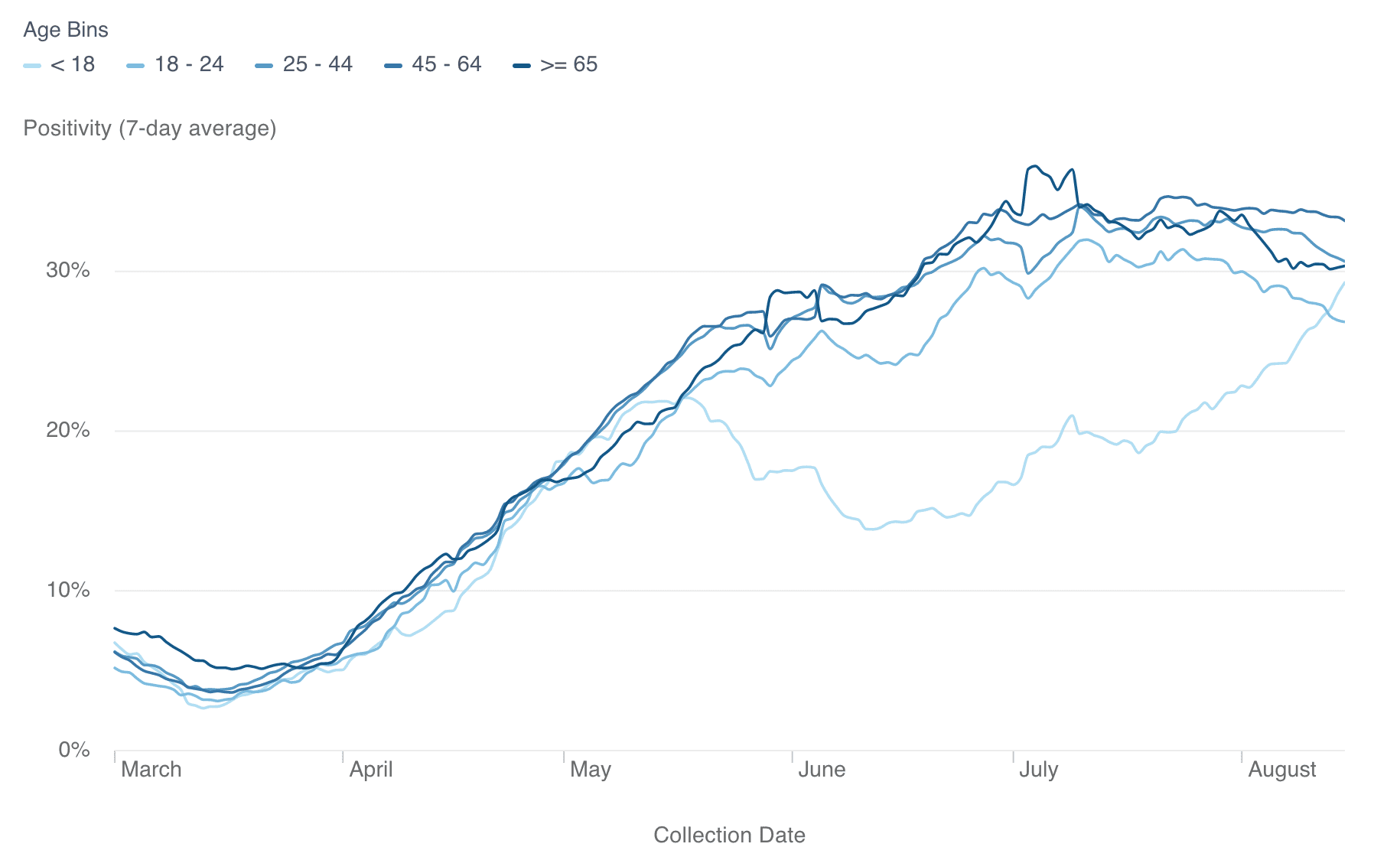
The FDA has said that they’ll be using nonclinical data, along with knowledge about the safety and efficacy of mRNA platforms to authorize bivalent boosters (which are a mix of two versions of the vaccine) in the fall. As we work with more health systems to bring phenotypic and genotypic data together, we’re excited about what that will mean for our ability to collect real-world evidence on vaccine efficacy.
